| Table of Contents |  |
|
Case Report
| ||||||
| Portal vein thrombosis after robot-assisted laparoscopic Roux-en-Y gastric bypass | ||||||
| Ranjodh Singh1, Randeep Badwal2, Hassan Shahid3, Elliot J Fegelmen4 | ||||||
|
1MD, Surgery Resident, Surgery Department, The Jewish Hospital, Cincinnati, Ohio, USA.
2MD, Medical Student, Surgery Department, The Jewish Hospital, Cincinnati, Ohio, USA. 3MD, Medical Student, Surgery Department, The Jewish Hospital, Cincinnati, Ohio, USA. 4MD, Attending Surgeon, Surgery Department, The Jewish Hospital, Cincinnati, Ohio, USA. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Singh R, Badwal R, Shahid H, Fegelmen EJ. Portal vein thrombosis after robot-assisted laparoscopic Roux-en-Y gastric bypass. Edorium J Gastrointest Surg 2014;1:1–4. |
|
Abstract
|
|
Introduction:
Portal vein thrombosis after gastric bypass has been rarely described in medical literature. It is a multifactorial occurrence, one related to surgical technique as well as predispositions to thrombosis in the patient. Nonetheless, it is one with deadly consequences if not diagnosed and treated promptly. The patient exhibited vague abdominal symptoms at presentation and was diagnosed with portal vein thrombosis via abdominal computed tomography.
Case Report: Herein, we discuss a case of a 40-year-old female, with an undiscovered Leiden V mutation and positive lupus anticoagulant, presented with portal vein thrombosis two weeks after robot-assisted laparoscopic gastric bypass and successful discharge. Conclusion: A clinician managing a postoperative laparoscopic Roux-en-Y gastric bypass patient should be aware of the possibility of portal vein thrombosis, and the precipitating factors predisposing patients to this condition. | |
|
Keywords:
Portal vein thrombosis, Gastric bypass, Laparoscopic bypass
| |
|
Introduction
|
|
Patients who undergo laparoscopic Roux-en-Y gastric bypass (LRYGB) usually have shorter length of stay and lower complication rates compared to open procedures. These advantages have also been clinically demonstrated in robot-assisted LRYGB, with non-inferior results [1] [2] [3]. Usually, complications of laparoscopy are minimal compared to their open counterparts, mainly associated with trocar insertion and abdominal insufflation (Figure 2) (Figure 3). Portal vein thrombosis (PVT) is an extremely rare but potentially fatal complication of LRYGB. As of 2009, there were a total of seven reported cases [1] [4] [5]. We are reporting our first case of PVT after robot assisted LRYGB. Features of the laparoscopic procedure itself may be responsible for this occurrence, in addition to pre-existing risk factors in the patient. |
|
Case Report
|
|
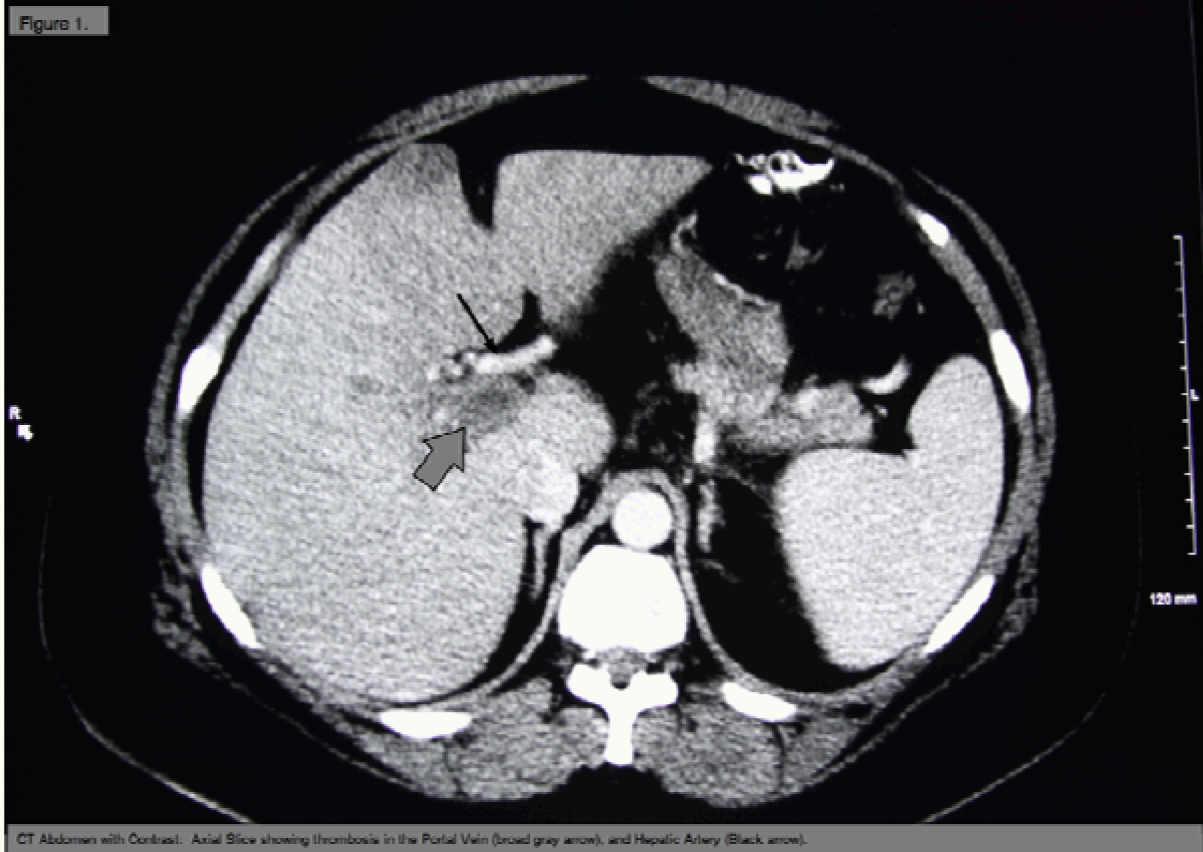
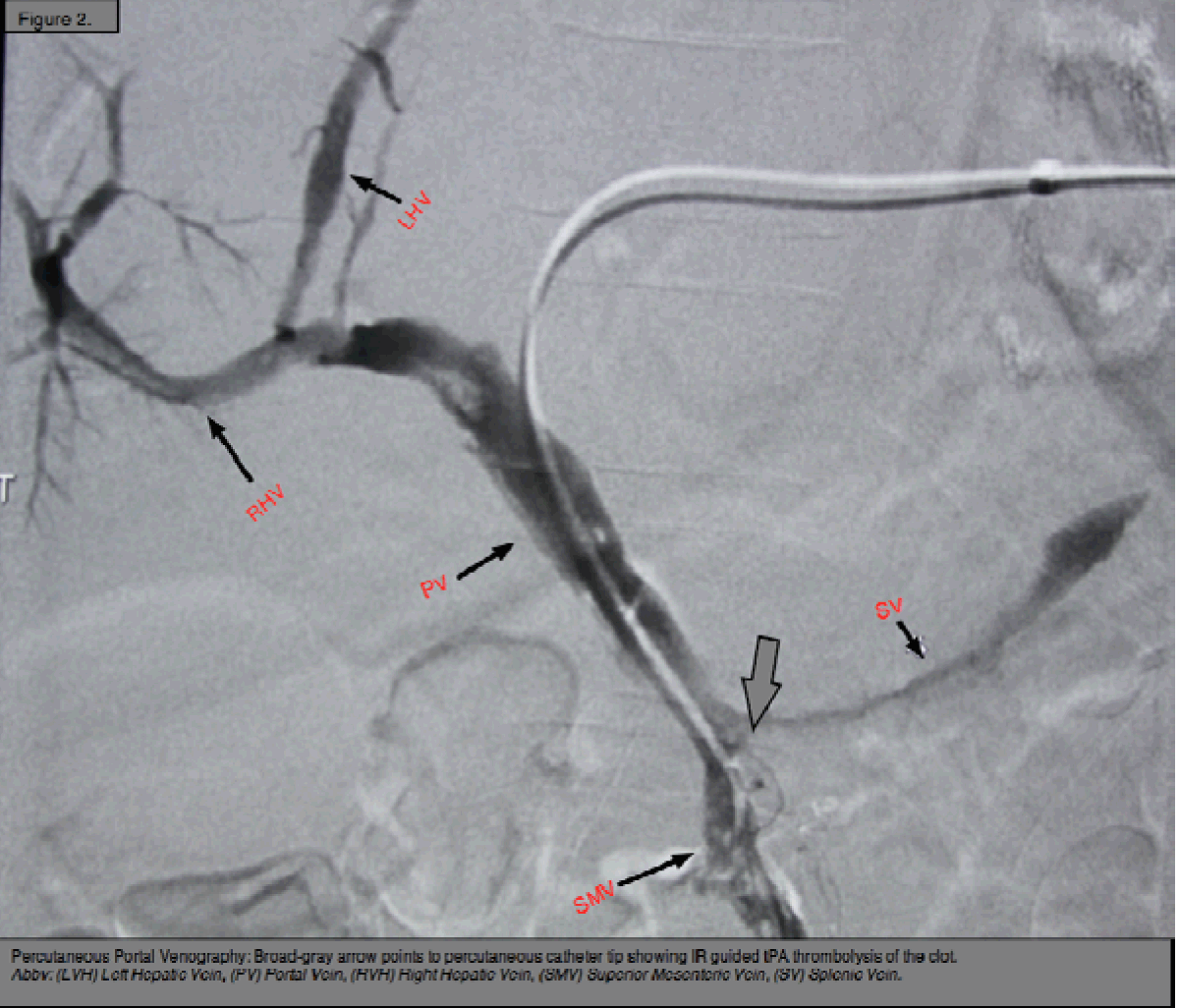
A 43-year-old female with a body mass index 36 kg/m2 and a history of hypothyroidism and migraine headaches, presented to our institution to undergo robotic-assisted LRYGB. Preoperative INR was 1.1 and institution standard coagulation prophylaxis of subcutaneous 5000 IU heparin was administered. During the procedure access to the abdominal cavity was gained using long shaft (150 mm) port for camera visualization. After access standard port placement for robotic assist proceeded under direct visualization. The Roux limb was created using GIA-staple for division. The jejunum-jejunal anastomosis was created using side-to-side stapling technique and gastric-jejunum anastomosis was sewn using 3-0 vicryl sutures. Gastric end was also sewn using 3-0 vicryl line. No injuries to any structures were noted and no unusual findings were noted during the procedure. Total operative time was 2 hours and 10 minutes including robot docking and skin closure. Subcutaneous heparin (5000 IU every 8 hours) was continued for the duration of her stay. She tolerated the procedure without complication and the patient was discharged postoperative day after successful oral intake. Postoperative day 14, the patient presented to our emergency department with a 6-day history of right upper quadrant tenderness and emesis. She denied dysuria, hematuria, diarrhea or bloody bowel movements and reported normal fluid intake until the onset of symptoms. Physical examination revealed right upper quadrant abdominal tenderness and hypoactive bowel sounds, without peritoneal signs or distension. The trocar incision sites were well healed. The rest of the examination were unremarkable. Laboratory studies showed an elevated leukocyte count of 12.4 mm3 (normal range: 4500–11,000 mm3) and a lipase of 761 U/L (normal range: 18–180 U/L). Electrolytes, liver function tests, and urine analysis were normal. A diagnosis of acute pancreatitis was made and a confirmatory abdominal computed tomography (CT) scan (Figure 1) was done, which showed possible thrombosis of the portal vein, later confirmed with a venogram (Figure 2). Coagulation disorder workup revealed that the patient possessed a heterozygote factor V Leiden mutation and also positive for lupus anticoagulant. Directed tissue plasminogen activator thrombolysis was initiated by interventional radiology with continued anticoagulation on heparin drip bridged to coumadin, with complete resolution. She was conservatively managed for concomitant pancreatitis over 21 days, and discharged upon a therapeutic INR and oral intake toleration. |
|
|
|
|
|
Discussion
|
|
The development of PVT can be simplified to Virchow's triad consisting of stasis, trauma and hypercoagulability. Reduced venous flow in large vessels due to pneumoperitoneum, a decrease in surface area and hence reduced endothelial cell surface-to-blood volume ratio, and intrinsic trauma secondary to manual manipulation and surgical technique, are contributors to this triad [6] [7]. Abdominal insufflation with carbon dioxide is routinely employed in laparoscopy as standard procedure. Studies have demonstrated that portal blood flow decreases as much as 53% from baseline with 14 mmHg of insufflation pressure. In addition, mesenteric vasoconstriction results from hypercapnia related to intraperitoneal carbon dioxide absorption, described in experimental animal models [4] [5]. Lesser factors that favor thrombosis by interrupting flow include the reverse Trendelenburg position [8]. In our patient, a standardized 15 mm/Hg of carbon dioxide insufflation in combination with reverse Trendelenburg position were utilized. Repair of the Petersen defect created after anastomosis of the roux limb is specific to gastric bypass. Here, surgical technique can initiate a thrombotic event. In repairing the Petersen defect or jejunal Roux limb mesentery defect, a misplaced suture may inadvertently interrupt the venous outflow forming a nidus for thrombosis [5]. Goitein et al. eluded to a compression or contact of the splenic vein causing intimal damage as a precipitant of portomesenteric thrombosis following LRYGB in their retrospective review of 17 cases of portomesenteric thrombosis [9]. However, venous flow interruption is not readily verifiable during surgery. They further postulated a reduced fluid intake (<2 L/day) and change in blood flow due to interruption of short gastric vessels as a possible cause for portomesenteric thrombosis [9]. In this case, a specific fluid intake was not calculated by the patient and thus a comment cannot be made on whether this was an additional cause for thrombus formation in our patient. Predisposition to hypercoagulability in our patient consisted of morbid obesity, heterozygous factor V Leiden mutation, positive lupus anticoagulants, and pancreatitis. Obesity promotes thrombosis through a variety of mechanisms, including adipocytokines, depression of the fibrinolytic cascade and augmentation of the coagulation cascade, increased inflammation, and endothelial dysfunction [8] [9] [10]. Factor V Leiden, a gain-of-function mutation, has been shown to increase the relative risk of thrombosis to 7.9, for heterozygous mutants [11]. In addition, lupus anticoagulants antibodies targets apolipoprotein H, prothrombin, and annexin V; which are natural inhibitors of thrombosis [12]. Finally, it is unclear how PVT and pancreatitis may be related in this patient. Gonzalez et al. report a 1–2% incidence of splanchnic vein thrombosis in severe acute pancreatitis, postulating direct compression of the portal vein by and inflamed pancreas [13]. There were no clear indications of such and entity on imaging, in our patient. |
|
Conclusion
|
|
This case offers multiple points of interest in improving patient care. Portal vein thrombosis (PVT) is an uncommon differential of this presentation, and was diagnosed incidentally on computed tomography (CT) scan. Further investigation revealed a multifactorial predisposition to hypercoagulability, including heterozygous Leiden V, and lupus anticoagulant. The patient later revealed a family history of a sister with a Leiden V diagnosis and multiple failed pregnancies in a follow-up interview. Specific questions about family history in preoperative work-up may have been overlooked. This patient's condition resulted from an accumulation of multiple constituents contributing to hypercoagulability. An in-depth detailed history with specific questions regarding coagulation disorder in patient's and familial history may help prevent a repeat occurrence. Patients should be thoroughly educated about postoperative red flag symptoms. Furthermore, a clinician managing a postoperative laparoscopic Roux-en-Y gastric bypass patient should be aware of the possibility of PVT, and the precipitating factors predisposing patients to this condition. |
|
References
|
|
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Ranjodh Singh – Conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Critical revision of the article, Final approval of the version to be published Randeep Badwal – Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Hassan Shahid – Acquisition of data, Drafting the article, Critical revision of the article, Final approval of the version to be published Elliot J Fegelmen – Analysis and interpretation of data, Critical revision of the article, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2014 Ranjodh Singh et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|